Resurrection on Repeat: Rules and Orders of the Humane Society (1787)
To bring the deceased back to life, especially those taken before their time, has long been a dream of legends and myth. In the case of the “apparently drowned”, however, it is possible to perform the seemingly miraculous and restore a limp body to full animation before lethal asphyxiation occurs. Yet despite the relatively simple techniques needed to perform this operation, they have taken millennia to develop. Early representations of resuscitation are shallow in information. Some scholars point to the Battle of Kadesh, as depicted at the Egyptian Ramesseum, where the drowned Hittite Emperor is held upside down by his men; others to the Hebrew Book of Kings, where Elisha revives a dead child with his “mouth upon his mouth” as an example of artificial ventilation. The idiom “over a barrel” may point to a practice, possibly medieval in origins, for rolling an unconscious body on a cask until they cough up water (or it might equally suggest flogging). The history of modern resuscitation in Europe conjures, though did not coin, another idiom: “to blow smoke up your”. . . well, we all know where that leads. Driven by an Enlightenment humanitarianism, social reformers and physicians began addressing a leading cause of preventable expiration that had rarely been treated on a national scale — death by water.
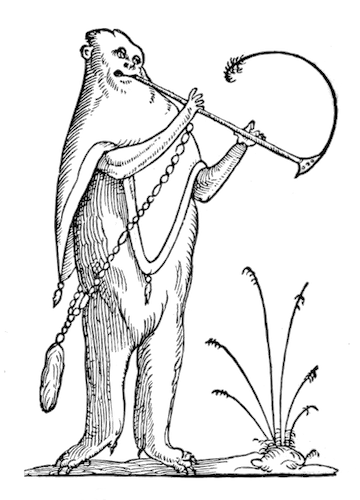
In the 1730s, René Antoine Ferchault de Réaumur popularized a recent discovery: the seemingly lifeless could be revived with a wealth of strategies. This “Pliny of the Eighteenth Century” (Réaumur invented a precursor to the Celsius scale, influenced methods of silk production in China, and pioneered the process of metallic tinning still used today) wrote a pamphlet titled Avis pour donner du secours à ceux que l’on croit noyez (Advice to aid those believed drowned). After debating the pros and cons of tickling the nose with feathers and filling a drowning man’s mouth with warm urine, Réaumur reveals what he believes to be the best technique: using a pipe stem to blow stimulating tobacco smoke into the intestines through the rectum. Louis XV found the pamphlet dazzling and encouraged its wide distribution. Startlingly, as Anton Serdeczny discusses in his recent book on reanimation, soon riverbanks across Europe were lined with “resuscitation kits”, as close-by as a contemporary defibrillator, which contained all the necessary supplies for giving a nicotine enema (and later, thankfully, included bellows as a substitute for breath).
The Most Effectual Method of Recovering a Drowned Person, a print made by John Fougeron, satirising the French technique, 1747 — Source.
The pamphlet above documents thirteen years of success since the 1774 establishment of Britain’s Humane Society for the Recovery of Persons Apparently Dead by Drowning (still in existence, with an expanded mission, today). Why was a society necessary for what many might do on impulse? Despite a wealth of new resuscitation methods, it was difficult to encourage public uptake (even the anatomist William Hunter, for instance, considered mouth-to-mouth breathing “vulgar”). Due to the taboo of touching corpses and a scientific/folk belief that once respiration ceased, so too fled the soul, the semi-drowned often suffocated while surrounded by their rescuers, who presumed them already gone. Also, many would-be lifeguards did not know how to swim. The Humane Society in London was created after Dutch physicians, inspired by Réaumur, established a society in Amsterdam, where canal drownings were plentiful, offering educational information and paying “premiums to those who saved the life of a citizen in danger of perishing by water”. The success of this society, evidenced by its proceedings, encouraged similar social programs across Europe. In Britain, an English translation was commissioned by William Hawes and Thomas Cogan, who founded the Humane Society soon after, announcing “The Plan” in a 1774 pamphlet.
By 1787, the Society was able to show results — 897 lives saved — and, in the rhetoric of welfare statehood, deemed itself a “great public utility”. The pamphlet contains the latest “plain Methods of Treatment” to recover the drowned. First remove the clothes and replace them with the great-coats of bystanders. Then move the body to the nearest pub, preferably with a good fire in winter months. One person should blow bellows into a nostril, closing the other, so that “the noxious and stagnant vapours will be expelled, and natural breathing imitated”, while a second person rhythmically compresses the chest. What, for a moment, resembles contemporary CPR, then takes a culinary turn. Next, rub the body with salt and spritz it with rum: hot brandy should be applied to the stomach and loins when needed and “the nostrils now and then tickled with a feather”. Here comes the tobacco: “fumes should be thrown up the fundament”, continuously, while making sure to shake the body every so often. Should all else fail, the society recommends electrocuting the corpse — a technique only to be tried by “the judicious and skilful”. Never bleed the body.
The rest of the pamphlet is packed with eye-witness testimonies of resuscitation. While the techniques are not quite those we use today, they seemed to get results, and were frequently reprinted in The Gentleman’s Magazine and other periodicals. Yet the Humane Society’s greatest tool may have been financial incentive: two guineas for attempted rescues in the Westminster area; four guineas per successful resuscitation; and a guinea to the pub for providing premises. Not only were the seemingly-drowned experiencing novel treatments, more bodies were being pulled out of the waters than ever before.
While it is easy to laugh at the idea of a tobacco smoke enema, resuscitation practices continue to be refined — what saves lives today, may soon be antiquated. In 1906, Sydney Holland, President of the Life-Saving Society, fatally ruptured the spleen of a young woman by using the “Silvester Method”, which required four people to lift the arms and apply chest pressure, prompting him to encourage the “Schäfer Method”, where the body is placed face-down and the thorax compressed, which he subsequently propagated throughout the British Empire. The same networks that allowed Holland to disseminate reforms had been used to extract knowledge and medicines for centuries. During the colonial period when non-Western healthcare was systematically dismissed and suppressed as irrational and superstitious, indigenous techniques were refashioned as European. In 1891, physicians were inspired after a man in Australia was restored by a smoky fire, “a native method”. And the tobacco enema, requiring a New World crop, tracks back to the practices of indigenous peoples across North and South America, described by John Tennant, who controversially adapted these herbal remedies in The Poor Planter’s Physician (ca. 1727), more than a decade before Réaumur published his treatise.
Enjoyed this piece? We need your help to keep publishing.
The PDR is a non-profit project kept alive by reader donations – no ads, no paywalls, just the generosity of our community. It’s a really exciting model, but we need your help to keep it thriving. Visit our support page to become a Friend and receive our themed postcard packs. Or give a one-off donation. Already a supporter? A huge thank you for making all this possible.
Jan 19, 2022